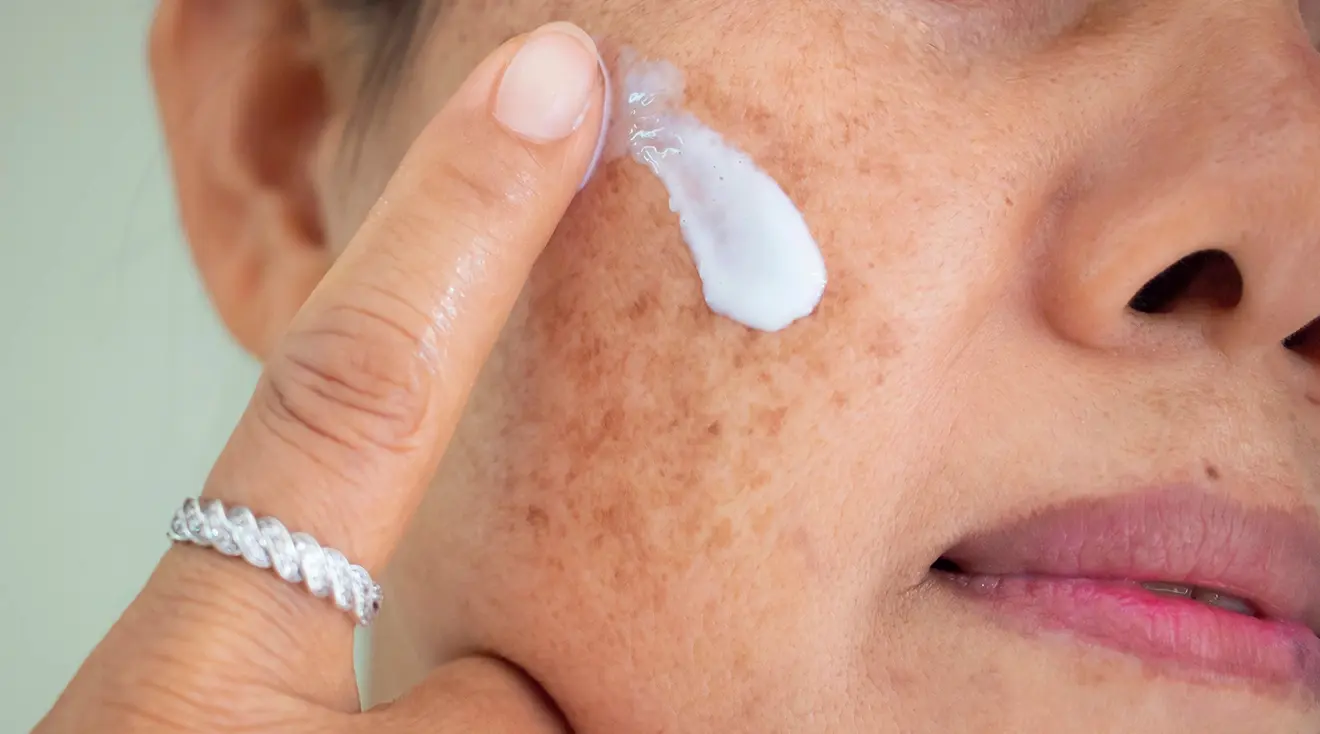
Melasma is a common form of hyperpigmentation that appears as brown or greyish patches on the skin, most often affecting the cheeks, forehead, nose, and upper lip. It is frequently referred to as “the mask of pregnancy” because it commonly develops during pregnancy due to hormonal changes. In sunny environments like Singapore, where ultraviolet (UV) exposure is high year-round, melasma tends to be even more prevalent and noticeable among expectant mothers.
While the condition is harmless, many patients seek ways to manage or treat melasma safely without affecting their pregnancy. In this article, we will explore the causes of melasma during pregnancy, important safety considerations, and the treatment options available both during and after pregnancy.
What Causes Melasma During Pregnancy?
Melasma during pregnancy is primarily driven by hormonal changes, particularly the increase in estrogen and progesterone levels. These hormones stimulate melanocytes (the cells responsible for producing pigment), leading to excess melanin formation in certain areas of the skin. As a result, uneven patches of pigmentation begin to appear, most commonly on sun-exposed areas of the face.
In addition to hormones, sun exposure plays a significant role in triggering and worsening melasma. Ultraviolet (UV) rays stimulate pigment production, which is why the condition is more noticeable in tropical climates like Singapore. Even brief daily exposure—such as walking outdoors or sitting near windows—can contribute to its development.
Other contributing factors include genetic predisposition and skin type. Individuals with darker skin tones or a family history of pigmentation are generally more prone to developing melasma. The condition typically appears on areas such as:
- Cheeks
- Forehead
- Upper lip
- Bridge of the nose
Understanding these underlying causes is important, as it helps guide safer and more effective ways to manage melasma during pregnancy.
Why Treating Melasma During Pregnancy Requires Caution
While melasma is harmless, treating it during pregnancy requires careful consideration. Many standard pigmentation treatments are not recommended for expectant mothers because the skin becomes more sensitive and reactive during pregnancy, increasing the risk of irritation or adverse effects.
Moreover, some commonly used ingredients and procedures for melasma, such as retinoids, hydroquinone, and certain chemical peels, may pose potential risks to the developing baby. Even laser and energy-based treatments are generally postponed until after pregnancy due to limited safety data.
Because of these factors, it is crucial for pregnant women to prioritise safe management strategies and consult a qualified doctor before attempting to treat melasma. Focusing on prevention and gentle, pregnancy-safe options ensures both maternal and fetal well-being while helping to minimise the appearance of pigmentation.
Safe Melasma Management During Pregnancy
Although aggressive treatments are generally avoided during pregnancy, there are several safe strategies to help manage melasma and prevent it from worsening. Sun protection is the most important step, as UV exposure can significantly intensify pigmentation. Pregnant women should use a broad-spectrum sunscreen with SPF 30–50+, reapply frequently, and combine it with physical barriers such as wide-brimmed hats or umbrellas.
A gentle skincare routine is also recommended. Avoid harsh exfoliants or strong bleaching agents that can irritate sensitive skin. Pregnancy-safe topical ingredients can be helpful, including:
- Azelaic acid – a mild and safe pigment reducer
- Vitamin C – an antioxidant that brightens skin and helps reduce pigmentation
Introducing new products gradually and monitoring skin reactions is key. While these measures may not completely remove melasma, they help control its severity and reduce the risk of further darkening.
Treatments to Avoid During Pregnancy
During pregnancy, it’s important to know which melasma treatments are unsafe or not recommended, as they can pose risks to both mother and baby. Common treatments to avoid include:
- Retinoids (e.g., tretinoin) – can cause developmental risks if absorbed systemically
- Hydroquinone – typically avoided due to limited safety data and potential systemic absorption
- Oral medications for pigmentation – most are contraindicated during pregnancy
- Laser and energy-based treatments – generally postponed until after pregnancy because of unknown effects on fetal health
Consulting a qualified doctor before attempting any treatment is essential. Even seemingly mild procedures or over-the-counter creams may not be safe. Prioritising pregnancy-safe approaches ensures you manage melasma effectively without compromising maternal or fetal health.
Will Melasma Go Away After Pregnancy?
Many cases of pregnancy-related melasma improve naturally after delivery, as hormone levels gradually return to normal. For some women, the pigmentation may fade significantly within a few months, while for others, it can persist for longer or become more noticeable with sun exposure.
It’s important to understand that sun protection remains essential even after pregnancy, as UV rays can trigger new pigmentation or darken existing patches. While melasma may improve on its own, some individuals may still require treatment postpartum to achieve a more even skin tone. Setting realistic expectations helps patients understand that improvement is possible, but complete resolution is not guaranteed for everyone.
Post-Pregnancy Treatment Options for Melasma
Once pregnancy is over, and depending on whether you are breastfeeding, more treatment options become available to effectively address melasma. These include:
- Medical-grade topical treatments: Prescription creams containing safe depigmenting agents can help lighten persistent patches.
- Chemical peels: Superficial peels can improve skin texture and reduce pigmentation when performed by a trained professional.
- Laser treatments: Certain lasers and light-based therapies can target stubborn pigmentation, but require proper assessment to ensure suitability for your skin type.
A personalised treatment plan is crucial, as the severity of melasma and skin sensitivity vary from person to person. Working with a qualified aesthetic doctor ensures that the chosen approach is safe, effective, and tailored to your specific needs.
Summary
Melasma during pregnancy is common and usually harmless, but it can be distressing for many women due to its visible appearance. Understanding the causes, practicing sun protection, and using pregnancy-safe skincare can help manage the condition until more targeted treatments are possible after delivery.
With the right care, you can reduce pigmentation, protect your skin, and achieve a more even complexion over time. If you are concerned about melasma or want guidance on safe treatment options during or after pregnancy, contact our specialists at:
Harmony Aesthetics Clinic – Titanium Lifting | Sofwave | Ultherapy | Freckles | Melasma Treatment Singapore
〒239693, Grange Rd, 1号, Orchard Building, #13-01
Phone: (65) 6970 5418